Introduction
The phrase 'high-risk pregnancy' is one that stops most families in their tracks. It sounds alarming, and the uncertainty that follows a doctor using those words can be more difficult to manage than the medical reality behind them.
Understanding what the term actually means, what it implies, what it does not imply, and what it requires replaces that uncertainty with something more useful. Most high-risk pregnancies, managed with appropriate care, end with healthy mothers and healthy babies.
What High-Risk Actually Means
A pregnancy is classified as high-risk when factors are present that increase the probability of complications for the mother, the baby, or both. That classification is not a prediction of a poor outcome. It is a signal that closer monitoring is necessary, more frequent appointments, additional scans, and earlier intervention if specific thresholds are crossed.
The factors that create this classification vary widely. Maternal age under eighteen or over thirty-five increases certain risks. Pre-existing conditions like diabetes, hypertension, thyroid disorders, or autoimmune conditions require more careful management during pregnancy than they do outside it. Multiple pregnancies carry inherent additional complexity. A history of previous pregnancy loss, preterm birth, or caesarean delivery also places a subsequent pregnancy in a higher monitoring category.
None of these factors mean a complication will occur. They mean the medical team needs a fuller picture, more frequently, to catch anything developing before it becomes serious.
Common Complications That Require Monitoring
Gestational hypertension and pre-eclampsia elevated blood pressure developing during pregnancy are among the most common high-risk conditions managed by obstetric teams. Left unmonitored, they can progress rapidly. Identified early through regular blood pressure checks, they are managed effectively through medication, dietary adjustment, and carefully timed delivery planning.
Gestational diabetes develops in women with no prior diabetic history and resolves after delivery in most cases. It requires dietary management and blood sugar monitoring throughout the pregnancy to protect foetal growth and reduce pregnancy complications.
Preterm labour risk, placenta previa, and foetal growth restriction are conditions that regular scanning identifies and that clinical teams at a high risk delivery hospital are equipped to manage with protocols specifically designed for each situation.
Meera's blood pressure elevated during her second trimester without obvious symptoms. Her routine appointment caught it. Her care team adjusted her monitoring schedule, began medication, and planned her delivery timeline accordingly. She delivered at term without complication, an outcome that required catching the issue at the right moment.
What Treatment Actually Involves
High risk pregnancy treatment in Rajkot specialists provide is not dramatically different from standard obstetric care in its fundamentals. It is more frequent, more detailed, and more responsive.
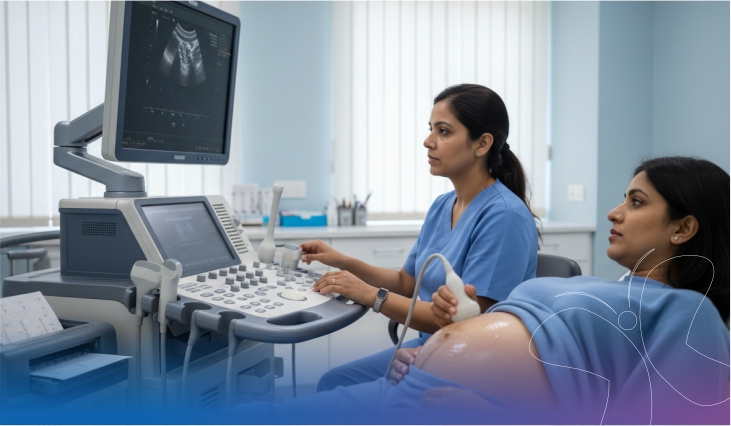
Appointments happen more often. Scans measure foetal growth and fluid levels at intervals that standard pregnancies do not require. Blood pressure, blood sugar, and specific protein levels are monitored against thresholds that trigger action when crossed. Some women require periods of bed rest. Some require hospitalisation in the final trimester for continuous monitoring.
The goal at every stage is the same: maintain conditions that support the pregnancy as close to term as possible, intervene at the earliest point that intervention improves the outcome, and have the surgical and neonatal capability ready if delivery needs to happen quickly.
Choosing a pregnancy specialist in Rajkot with specific experience in high-risk cases rather than a general practitioner or a facility without advanced obstetric infrastructure makes a measurable difference in how effectively these pregnancies are managed.
How Families Can Support the Process
Follow every instruction the medical team provides without treating any as optional. Medication schedules, dietary restrictions, activity limitations, and rest requirements are not conservative suggestions; they are clinical decisions based on the specific risk profile of that pregnancy.
Attend every appointment without exception. High-risk monitoring only works when the data is current. A blood pressure reading from three weeks ago does not tell a doctor what is happening today.
Communicate openly about symptoms that change headaches, visual disturbances, swelling, reduced foetal movement, or anything that feels different from the previous day. These observations are clinically valuable and belong in the consultation room, not dismissed at home.
Conclusion
A high-risk classification changes the management of a pregnancy, not its ultimate potential. With the right pregnancy care in Rajkot specialists provide, consistent monitoring, and honest engagement between families and medical teams, the vast majority of high-risk pregnancies produce the outcome every family is working toward.
Stay informed. Attend every appointment. Choose care based on clinical capability. Trust the process and the team delivering it.