Introduction
No two pregnancies are identical, but the broad progression across nine months follows a pattern that every expecting mother benefits from understanding before she is inside it. Each trimester brings distinct physical changes, distinct nutritional demands, and distinct clinical priorities. Knowing what is coming rather than reacting to each development as it arrives makes the entire experience steadier, more confident, and considerably less anxious.
Month One and Two — Before It Shows
The earliest weeks of pregnancy are often the most disorienting because the changes happening internally are significant while the visible evidence remains minimal.
Fatigue in the first weeks is profound and often surprising in its intensity. It reflects the body's enormous energy investment in establishing the placenta and beginning foetal development. Rest is not optional during this period, it is physiologically necessary.
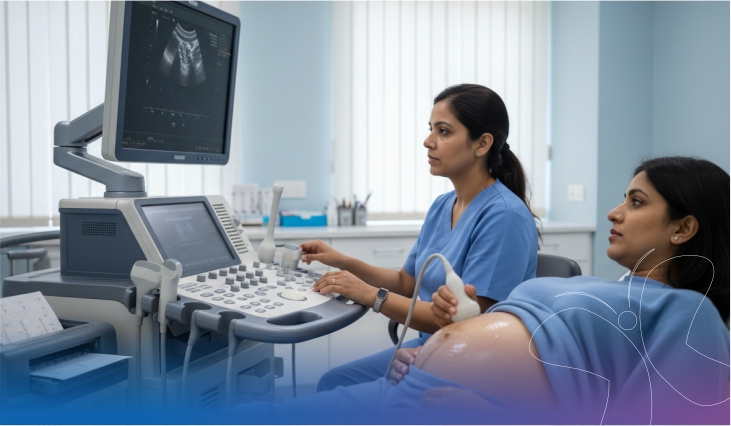
Nausea typically begins around week six and peaks around week nine for most women. Small, frequent meals and consistent hydration manage it more effectively than waiting until hunger becomes urgent. The first medical appointment should happen as early as possible; blood tests, baseline blood pressure, and early foetal confirmation establish the reference points that all subsequent monitoring builds on.
Month Three — The First Trimester Closes
By the end of the third month, the risk of miscarriage drops significantly, and most women begin to feel the worst of early pregnancy symptoms easing. Energy starts returning, and nausea gradually reduces for the majority.
This is the month when the full first-trimester screening is completed: nuchal translucency scan, blood tests for chromosomal markers, and assessment of foetal growth and heartbeat. These are not routine formalities. They are clinically significant assessments that inform the rest of the pregnancy's management.
Months Four to Six — The Middle Passage
The second trimester earns its reputation as the most comfortable phase. Nausea has usually resolved, energy has returned, and the pregnancy becomes visibly apparent. Foetal movements begin initially with subtle flutters, then increasingly definite kicks that become a reliable indicator of foetal wellbeing.
Appointments during this trimester screen for gestational diabetes, anaemia, and foetal anomalies. The anatomy scan around twenty weeks provides a comprehensive assessment of baby development stages. These appointments deserve the same attendance priority as first-trimester ones; conditions that develop silently during this phase are reliably caught through monitoring and easily missed without it.
Light physical activity, walking, swimming, and prenatal yoga is genuinely beneficial during these months. It supports cardiovascular health, manages weight gain, improves sleep, and prepares the body for the physical demands of labour.
Following sound 9 month pregnancy care tips across this trimester means maintaining nutritional consistency – iron, calcium, protein, and hydration – not just when symptoms prompt attention but as a daily, non-negotiable habit.
Months Seven to Nine — Preparation Becomes Concrete
The third trimester is where planning becomes action. The baby gains most of its birth weight during these weeks, and the body undergoes significant physical changes in preparation for labour. Breathlessness, back discomfort, frequent urination, and disrupted sleep are common and normal.
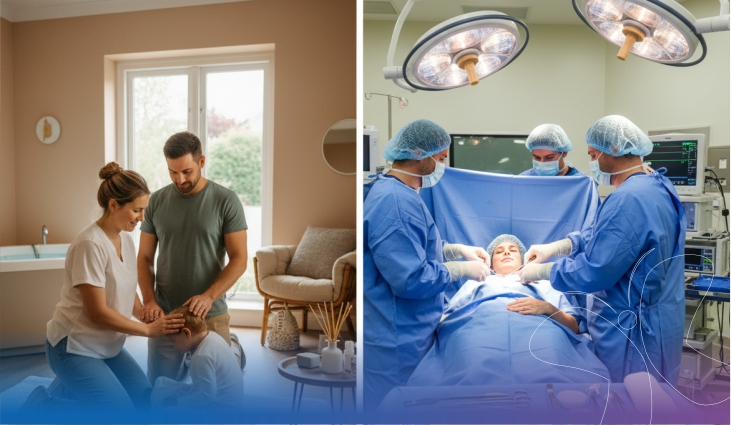
Appointment frequency increases fortnightly from month seven, weekly in the final month. Each visit monitors foetal position, fluid levels, blood pressure, and growth. These measurements together determine delivery timing and method.
Choosing a hospital during this trimester before labour begins is one of the most practical decisions a family makes. Understanding what maternity care Rajkot facilities offer in terms of obstetric team experience, emergency capability, and neonatal support allows a confident, considered choice rather than a pressured one.
Anjali researched her options at thirty weeks. She visited two hospitals, asked about their clinical teams, and chose based on the quality of answers she received rather than the appearance of the facilities. When her delivery date arrived, she was prepared not just physically but logistically and emotionally.
What Stays Constant Across All Nine Months
Attend every scheduled appointment without exception. The pregnancy month by month guide a clinical team follows is timed around specific developmental windows; missing appointments does not just delay information, it removes the opportunity to act on it at the right moment.
Eat with nutritional intention consistently. Sleep as much as the body requests. Communicate openly with your care team about every symptom, concern, and change in how you feel including emotional changes that many women underreport because they assume they are not relevant to an antenatal appointment.
Conclusion
Nine months of pregnancy care is not nine months of worry. It is nine months of informed, consistent attention to what the body needs and what the baby requires at each specific stage.
Following practical pregnancy health tips across all three trimesters – showing up to appointments, eating well, staying active within clinical guidance, and choosing a care team and hospital based on genuine quality – produces the outcome every family is working toward. The journey is demanding. With the right preparation, it is also entirely navigable.